Sleep disorders & brain health share a direct, measurable relationship. When your sleep breaks down, your brain pays the price first. About 70 million Americans have a chronic sleep disorder, per the American Sleep Association, and most don’t connect their daily cognitive struggles to their sleep pattern until significant damage has already occurred.
This article covers types of sleep disorders, how poor sleep damages the brain, what treatments actually work, and what you can do daily to protect your cognitive health.
Table of Contents
ToggleTypes of Sleep Disorders and Brain Effects
Types of sleep disorders and brain effects on the brain differ significantly by condition. Each disorder disrupts different stages of sleep and damages different brain systems. Getting the correct diagnosis determines whether treatment succeeds.
- Insomnia: About 10% of U.S. adults have chronic insomnia. It cuts slow-wave sleep, the phase where the brain clears beta-amyloid, a protein strongly linked to Alzheimer’s disease.
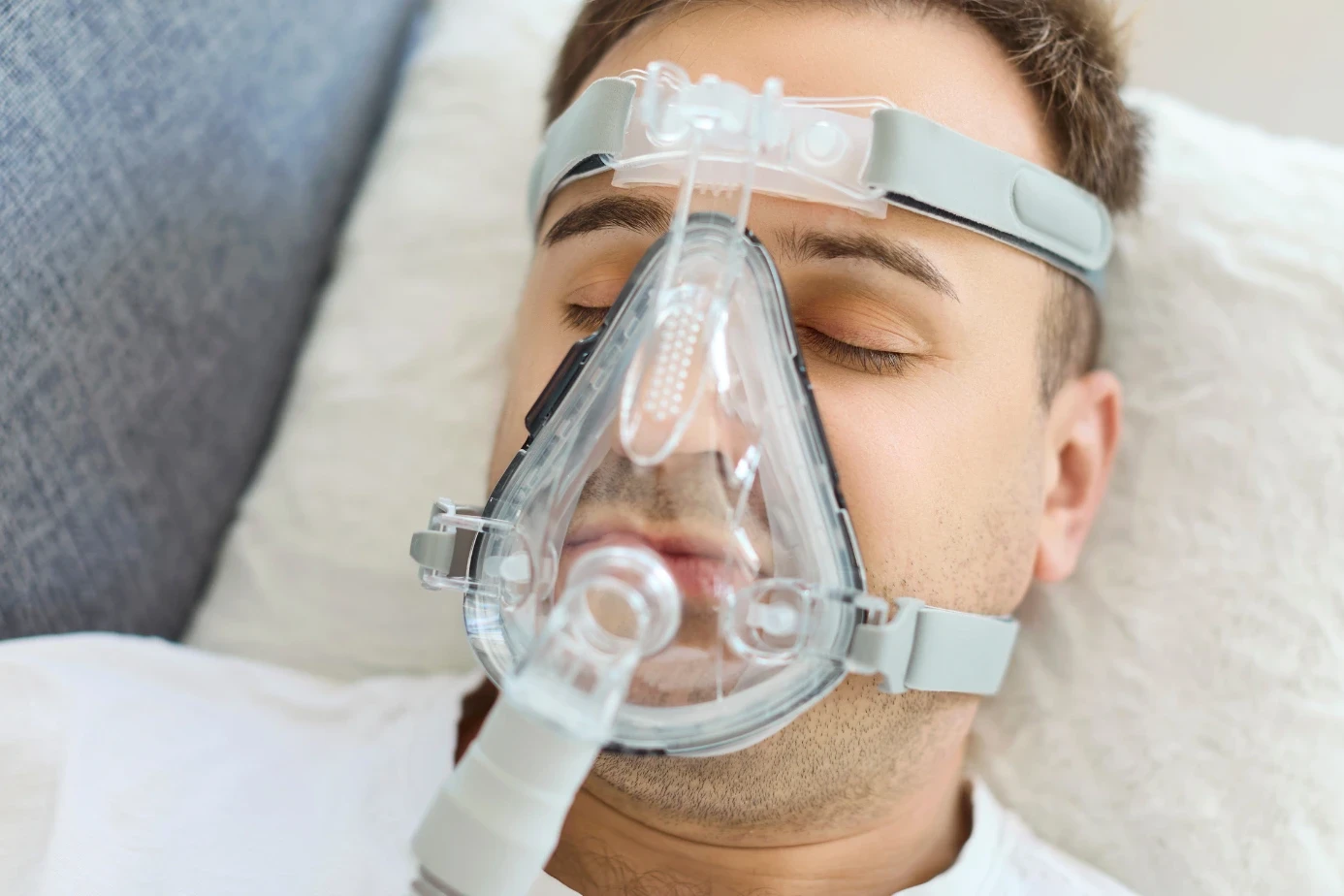
- Obstructive Sleep Apnea (OSA): The airway collapses during sleep. The brain experiences repeated oxygen drops throughout the night. University of California researchers found untreated OSA accelerates tissue loss in memory and attention regions of the brain.
- Restless Leg Syndrome (RLS): Creates uncomfortable sensations in the legs that prevent sleep onset. The brain stays in mild arousal all night, never entering deep recovery stages.
- Narcolepsy: A neurological disorder where the brain loses control of the sleep-wake switch. Hypocretin-producing neurons get destroyed, usually through an autoimmune process.
- Circadian Rhythm Disorders: The brain’s master clock, the suprachiasmatic nucleus, loses sync with natural light cycles. Night-shift workers in the U.S. carry the highest risk.
Sleep disorders & brain health are connected because the same brain regions that regulate sleep also control memory, emotion, and decision-making.
Impact of Poor Sleep on Brain Function
The impact of poor sleep on brain function shows up after a single bad night. Prefrontal cortex activity drops. Decision-making worsens. Impulse control weakens noticeably.
A study in Occupational and Environmental Medicine confirmed that 17 to 19 hours without sleep produces cognitive impairment equal to a 0.05% blood alcohol level. That is legally impaired driving territory.
Chronic sleep loss shrinks the hippocampus. A 2017 study in Nature Communications documented hippocampal atrophy in adults over 55 with consistently poor sleep. The hippocampus handles new memory formation. A smaller one means weaker learning capacity.
Sleep deprivation also raises cortisol chronically. High cortisol damages hippocampal neurons, deepens anxiety, and blocks emotional recovery.
During deep sleep, the brain’s glymphatic system activates and flushes metabolic waste, including tau protein, a known dementia marker. Harvard Medical School researchers confirmed this pathway. Without enough deep sleep, tau accumulates faster than the brain can remove it.
Memory Problems Due to Sleep Disorders
Memory problems due to sleep disorders are not simply forgetfulness. They are structural failures.
Memory consolidation requires two specific sleep phases: slow-wave sleep and REM sleep. During slow-wave sleep, the hippocampus replays the day’s events and transfers them to the neocortex for long-term storage. Skip that phase, and the transfer doesn’t complete.
A 2019 study in Current Biology found that a single night of REM disruption caused participants to misread neutral situations as threatening. The emotional memory system had no recovery window.
People with untreated sleep apnea score significantly lower on verbal memory and visuospatial tests compared to matched controls, per a meta-analysis in Sleep Medicine Reviews .
Memory problems due to sleep disorders get worse the longer the condition goes untreated. The hippocampal shrinkage from chronic poor sleep is measurable on MRI.
How to Improve Sleep for Brain Health
Improving sleep for brain health starts with sleep architecture, not just total hours. Behavioral changes produce results faster than most people expect.
- Fix sleep timing: The brain’s circadian clock stabilizes when you sleep and wake at consistent times daily, including weekends. It takes 2 to 3 weeks to reset.
- Cool the bedroom to 65 to 68°F: Sleep onset requires a 1 to 2°F drop in core body temperature. A warm shower 90 minutes before bed accelerates that drop.
- Cut blue light 90 minutes before bed: Harvard Health research found blue light suppresses melatonin by up to 50%. Melatonin signals the brain that sleep should begin.
- Time caffeine carefully: Caffeine has a 5 to 7 hour half-life. A 3 PM coffee still carries half its potency at 8 to 10 PM.
- Avoid alcohol within 3 hours of sleep: Alcohol fragments REM sleep. You fall asleep faster but lose the brain-restorative phases.
Improving sleep for brain health works best as a behavioral fix first. Medication addresses symptoms. Behavioral changes fix the system.
Treatments for Common Sleep Disorders
Treatments for common sleep disorders depend on accurate diagnosis. There is no universal approach.
- Insomnia: The American College of Physicians recommends Cognitive Behavioral Therapy for Insomnia (CBT-I) as the first-line treatment before any medication. CBT-I works in 70 to 80% of cases and produces lasting results without dependency risk. Most patients complete it in 6 to 8 sessions.
- Sleep Apnea: CPAP therapy keeps the airway open during sleep. Studies confirm CPAP reduces cardiovascular risk and slows cognitive decline in OSA patients.
- Restless Leg Syndrome: Check serum ferritin first. Levels below 75 mcg/L often drive RLS symptoms. Iron supplementation reduces symptoms in many patients. Dopamine agonists like pramipexole are prescribed for moderate to severe cases.
- Narcolepsy: Sodium oxybate (Xyrem) consolidates nighttime sleep and reduces cataplexy episodes. Modafinil manages daytime sleepiness effectively.
Daily Habits That Strengthen Brain Recovery During Sleep
Sleep quality determines how much actual brain repair happens each night.
Exercise increases slow-wave sleep by up to 15%, per research in Mental Health and Physical Activity . Morning or afternoon workouts perform best. Late-night exercise raises core body temperature and delays sleep onset.
Magnesium glycinate activates GABA receptors in the brain, the main inhibitory system that signals “slow down” for sleep. Around 48% of Americans are magnesium deficient. 300 to 400 mg before bed has clinical backing for improving sleep quality without sedation.
Consistent meal timing stabilizes secondary body clocks in the gut and liver, which feed signals back to the brain’s master clock. Irregular eating times disrupt that feedback loop.
Short naps of 20 minutes restore alertness without affecting nighttime sleep. Naps over 30 minutes push into slow-wave sleep and increase grogginess on waking.
Long-Term Strategies for Brain Health Through Sleep
Sleep debt partially recovers, but not completely. A study in Sleep showed that three recovery nights after five days of restriction only partially restored sustained attention. The deficit didn’t fully reverse. That result matters for anyone who normalizes chronic short sleep as manageable.
Wearables like Oura Ring and WHOOP track deep sleep and REM duration nightly. If deep sleep stays below 90 minutes consistently, that’s a clinical signal worth addressing with a sleep specialist, not just adjusting habits.
For adults over 55, the 2020 Lancet Commission on Dementia Prevention listed sleep disturbance as a confirmed modifiable risk factor. Treating it actually lowers dementia risk. That is not symptom management. That is prevention.
A polysomnography (sleep study) is the diagnostic standard for most sleep disorders in the U.S. Most major insurance plans cover it.
FAQs
How do sleep disorders affect brain function?
Sleep disorders & brain health data shows disrupted sleep blocks the glymphatic system from clearing toxic proteins, reduces prefrontal cortex output, and shrinks the hippocampus over time. Even two nights of poor sleep impairs cognitive performance to a measurable level equal to a 0.05% blood alcohol concentration.
Can poor sleep cause long-term brain damage?
Yes. Chronic sleep deprivation causes hippocampal atrophy, accelerates tau and beta-amyloid buildup, and raises dementia risk. A 2021 Nature Communications study found sleeping under 6 hours nightly between ages 50 and 60 correlated with a 30% higher dementia risk later in life.
Why does lack of sleep affect memory?
The brain transfers short-term memories to long-term storage during slow-wave sleep. Without it, that transfer fails. Memory problems due to sleep disorders are consolidation failures at the structural level, not temporary fogginess. One disrupted night measurably reduces next-day recall and learning speed.
What are the most common sleep disorders affecting the brain?
Chronic insomnia affects 10% of U.S. adults. Obstructive sleep apnea affects 26% of adults aged 30 to 70. Both impair memory, attention, and emotional regulation significantly. Circadian rhythm disorders, common in night-shift workers, follow closely in cognitive impact.
Can improving sleep reverse brain fog?
Yes, partially. Brain fog from short-term sleep loss clears within 2 to 3 full recovery nights. Structural damage from years of untreated apnea or insomnia takes considerably longer, and some changes may be permanent. Starting treatment early produces the most recovery.
How many hours of sleep does the brain need?
Adults need 7 to 9 hours, but architecture matters more than duration. The functional brain-health targets are 90 minutes of slow-wave sleep and 90 minutes of REM per night. A fragmented 7-hour night performs worse than a clean 6.5-hour night with full, uninterrupted cycles.
Does sleep apnea affect brain health?
Yes. Untreated OSA causes repeated oxygen desaturation events through the night, each stressing brain tissue. Long-term, this produces measurable white matter loss in attention and memory regions. CPAP therapy slows this damage and partially reverses cognitive decline in treated patients.
What is the best treatment for chronic insomnia?
CBT-I is the American College of Physicians’ first-line recommendation, ranked above all sleep medications. It outperforms sedatives in long-term results, carries zero dependency risk, and works in 70 to 80% of patients within 6 to 8 structured sessions.
Can sleep disorders lead to dementia?
Yes. The glymphatic system removes amyloid and tau during deep sleep. Chronic disruption allows these proteins to accumulate, the core biological mechanism of Alzheimer’s disease. The 2020 Lancet Commission confirmed sleep disturbance as a directly modifiable dementia risk factor, not just a symptom.
When should I see a doctor for sleep problems?
See a doctor after 3 weeks of poor sleep, loud snoring with pauses in breathing, daily unrefreshed waking, or worsening memory and focus. Sleep disorders & brain health damage accumulates silently before symptoms feel severe. Early diagnosis through a sleep study changes long-term outcomes significantly.
About The Author

Medically reviewed by Dr. Chandril Chugh, MD, DM (Neurology)
Dr. Chandril Chugh is a U.S.-trained, board-certified neurologist with expertise in diagnosing and managing neurological disorders, including migraines, epilepsy, Parkinson’s disease, and movement disorders. His clinical focus includes evidence-based neurological care and patient education.
All content is reviewed for medical accuracy and aligned with current neurological guidelines.