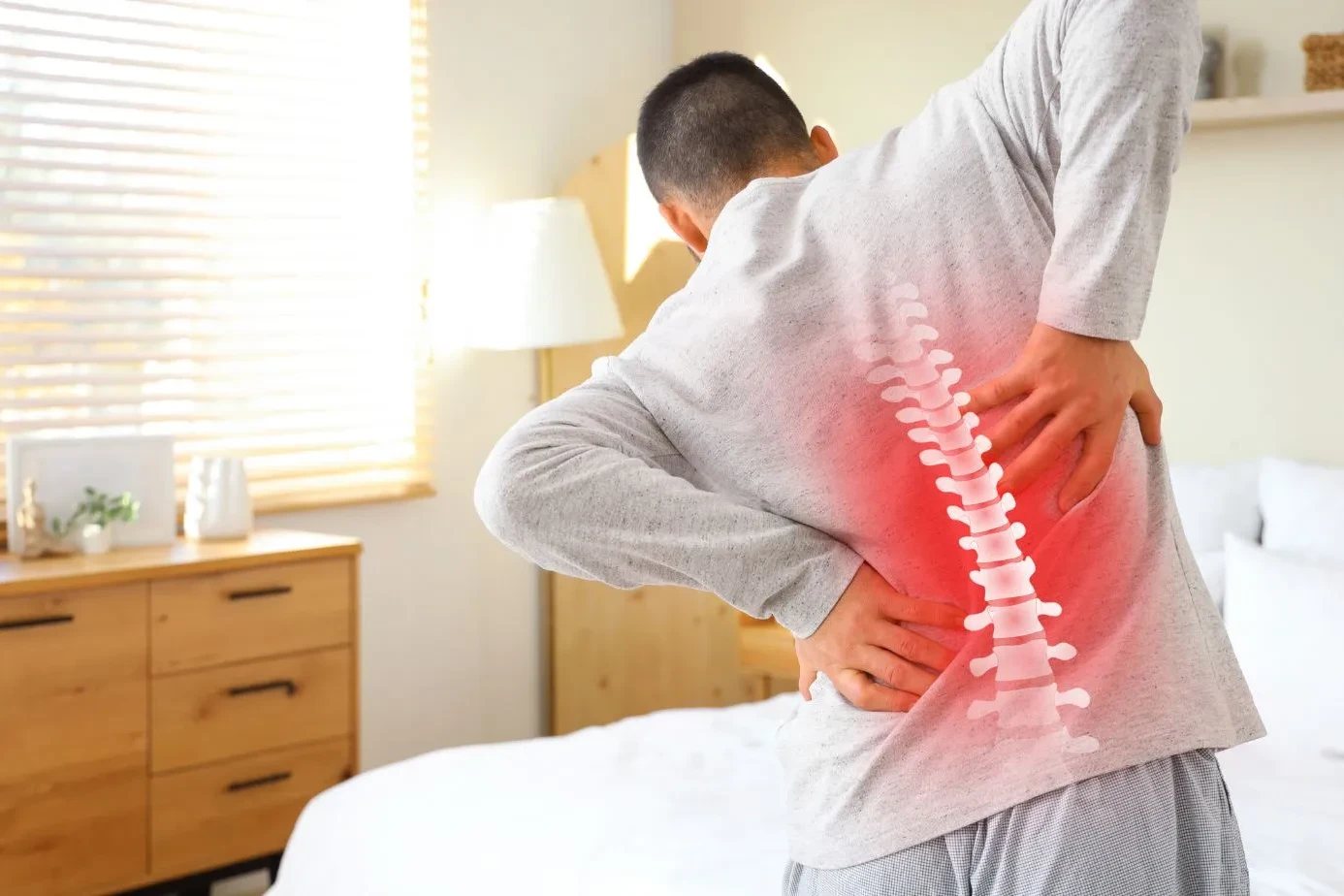
Neck pain at base of skull is pain felt where the back of your head meets the top of your neck. It often comes with tightness, pressure, or headaches that spread up over the head. Most cases trace back to muscle tension, poor posture, or nerve irritation, all of which respond well to targeted treatment.
This type of pain is increasingly common if you sit at desks, look at screens for hours, or carry stress in your shoulders. Left untreated, it builds into daily headaches and stiffness that limits movement.
Table of Contents
ToggleCommon Causes of Neck Pain at Base of Skull
Neck pain at base of skull has specific causes that most general neck pain articles skip. Knowing the exact source changes how you treat it.
Muscle Tension and Overuse
The suboccipital muscles sit at the base of your skull. There are four of them, and they control fine head movements. When they stay contracted for long periods, like during focused screen work or driving, they build up lactic acid and compress the nerves running through them. The result is deep, aching pain right at the skull base.
Poor Posture and Screen Use
When your head sits forward of your shoulders, the suboccipital muscles work double-time to hold it up. A head weighs roughly 10 to 12 pounds in neutral position. For every inch it shifts forward, the effective load on the neck muscles increases by about 10 pounds. Four inches forward means 50 pounds of load. That is what causes the grinding tightness at the skull base.
Cervicogenic Headache
This is a headache that starts in the neck, not the head. The C1, C2, and C3 nerve roots at the top of the spine share a pain pathway with the trigeminal nerve, which covers the head and face. When the upper cervical joints are stiff or irritated, pain refers up into the skull. It feels like a headache, but the real source is the neck joint.
Occipital Neuralgia
The occipital nerves run from the C2 spinal level through the suboccipital muscles and up the back of the head. When these nerves get compressed or inflamed, they produce sharp, shooting, or electric pain from the base of the skull to the top of the head and sometimes behind the eye. This is different from regular muscle tension pain and requires specific treatment.
Cervical Joint Dysfunction
The joints between C1 and C2 are the most mobile joints in the spine. Stiffness or minor misalignment here restricts head rotation and produces localized pain at the skull base. Physiotherapy manipulation targets these joints specifically.
Stress and Muscle Tension Neck Pain
Stress and muscle tension neck pain is one of the least-addressed causes online. When you are stressed, your body activates the fight-or-flight response. Shoulder and neck muscles contract involuntarily. The trapezius and levator scapulae tighten and pull on the muscles at the skull base. Chronic stress keeps these muscles in a semi-contracted state for hours or days.
Screen Time and Forward Head Posture Pain
Screen time and forward head posture pain is now one of the top causes of skull-base pain in people under 40. Most people are unaware that their head position, not their screen brightness or sitting duration, is the actual problem.
How Screen Use Affects Neck Alignment
When a screen sits below eye level, the head drops forward. When it sits too far away, the head juts forward to see better. Both positions shift the ear forward past the shoulder, which is the clinical definition of forward head posture.
Forward Head Posture Explained
In a neutral posture, your ear aligns directly above your shoulder. In forward head posture, the ear sits 2 to 4 inches in front of the shoulder. This position forces the suboccipital muscles into constant contraction to keep the head from falling forward, and the muscles at the front of the neck become weak from underuse.
Muscle Imbalance and Strain
The deep neck flexors (muscles at the front of the neck) become weak. The suboccipitals, upper trapezius, and levator scapulae become overloaded. This muscle imbalance is why stretching alone does not fix the problem. You need to both stretch the tight muscles and strengthen the weak ones.
Long-Term Effects on Spine
Research from the Journal of Physical Therapy Science shows that sustained forward head posture over months changes the curve of the cervical spine. The natural inward curve (lordosis) at the neck flattens or even reverses. This loads the discs, accelerates joint wear, and makes the entire neck more vulnerable to injury.
Symptoms Associated With Base of Skull Pain
Neck pain at base of skull produces a specific symptom cluster that differs from general neck pain:
- Dull, heavy pressure at the back of the head where it meets the neck
- Pain that worsens after prolonged sitting or screen use
- Headaches that start at the skull base and spread over the top of the head or behind one eye
- Stiffness when turning the head, especially to one side
- Tenderness when pressing on the muscles just below the skull
- Shoulder tightness on the same side as the head pain
- Occasional dizziness or blurred vision (in occipital neuralgia cases)
Stretches for Base of Skull Pain Relief
Stretches for base of skull pain relief work best when done consistently, not just when pain flares.
Chin Tucks
Pull your chin straight back, creating a double chin. Hold for 5 seconds. Repeat 10 times. This directly stretches the suboccipital muscles and resets the position of the head over the spine. Research supports chin tucks as the most effective single exercise for forward head posture correction.
Upper Trapezius Stretch
Sit upright. Drop your right ear toward your right shoulder. Reach your left hand down toward the floor to add gentle traction. Hold 30 seconds each side. This releases the upper trapezius, which often pulls tight at the skull base.
Levator Scapulae Stretch
Turn your head 45 degrees to one side. Drop your chin toward your armpit. Use one hand to gently pull the head further into the stretch. Hold 30 seconds. The levator scapulae runs from the shoulder blade to the upper cervical vertebrae. Tight levator scapulae is a very common overlooked cause of skull-base pain.
Neck Rotation Stretch
Slowly rotate your head left and right to the point of gentle tension, not pain. Hold each side for 10 seconds. Repeat 5 times. This mobilizes the C1-C2 joint, the main joint responsible for rotational movement.
Shoulder Blade Activation
Sit tall, pull your shoulder blades back and down together, and hold for 5 seconds. Repeat 15 times. Weak shoulder blade muscles force the upper trapezius to overwork, which feeds tension directly into the skull base.
Massage Techniques for Neck Pain
Massage techniques for neck pain at the skull base target specific muscles that most people do not know how to reach.
Self-Massage Techniques
Place both thumbs at the base of your skull, just beside the central ridge of bone. Apply firm pressure and make small circular movements. Work outward from the center. Spend 60 to 90 seconds on each side. This directly targets the suboccipital muscle group.
Trigger Point Release
A trigger point is a tight knot in a muscle that refers pain elsewhere. The suboccipital trigger points refer pain upward over the head and behind the eye. Press firmly on a tender spot and hold steady pressure for 30 to 90 seconds until the pain diminishes by about 50%. Do not rub. Hold and wait.
Foam Rolling for Upper Back
Foam rolling the thoracic spine (mid-back) indirectly reduces neck pain at base of skull because upper back stiffness forces the neck to compensate. Lie on a foam roller placed across the upper back. Support your head with your hands. Gently extend over the roller at each thoracic level for 30 seconds.
Professional Massage Therapy
A trained massage therapist using myofascial release techniques on the suboccipitals produces faster results than self-massage for chronic cases. Weekly sessions for 4 to 6 weeks combined with home stretching resolve most tension-based skull pain.
Stress and Muscle Tension Neck Pain
Stress and muscle tension neck pain creates a cycle: tension causes pain, pain increases stress, stress increases tension.
Stress Response and Muscle Tightness
Cortisol and adrenaline trigger muscle contraction as part of the stress response. In modern stress (work deadlines, anxiety), there is no physical action to release this contraction. The muscles stay tight. The suboccipitals, trapezius, and jaw muscles are the first to feel it.
Jaw and Neck Connection
The jaw (temporomandibular joint) and the upper cervical spine share muscle connections. People who clench their jaw during stress load the same muscles that attach to the skull base. Jaw clenching is a direct contributor to skull-base pain that almost no general article mentions.
Sleep and Stress Impact
Poor sleep from stress keeps cortisol elevated overnight. This means neck muscles do not fully relax during sleep. People with chronic stress wake with neck stiffness because their muscles never properly recovered during the night.
Relaxation and Breathing Techniques
Diaphragmatic breathing (deep belly breathing) activates the parasympathetic nervous system, the opposite of fight-or-flight. Five minutes of slow belly breathing reduces muscle tension measurably. Pair this with progressive muscle relaxation, where you contract and release each muscle group, for faster relief of stress and neck pain.
Medical Treatment Options
Pain Medications
Ibuprofen (400 to 600 mg) reduces both pain and inflammation at the neck joints. Acetaminophen works for pain only, not inflammation. For occipital neuralgia, regular NSAIDs do not address the nerve component; doctors prescribe gabapentin or amitriptyline instead.
Physical Therapy
A physiotherapist addresses the specific muscle imbalances driving the pain. Manual therapy to the upper cervical joints combined with deep neck flexor strengthening exercises produces results in 4 to 8 weeks for most patients with neck pain at base of skull.
Muscle Relaxants
Cyclobenzaprine or baclofen reduce acute muscle spasm. These are short-term tools, used for 5 to 7 days during severe flare-ups. They do not fix the underlying posture or muscle imbalance.
Nerve Blocks
For occipital neuralgia, an occipital nerve block injects local anesthetic and steroid directly into the greater occipital nerve at the skull base. Relief lasts weeks to months. This is both diagnostic (confirming occipital neuralgia) and therapeutic.
Interventional Pain Management
Radiofrequency ablation targets the C2-C3 facet joints for patients with cervicogenic headache that does not respond to other treatments. The procedure uses heat to disable the pain-carrying nerve fibers. Relief lasts 6 to 12 months before nerve fibers regenerate.
Preventing Recurring Neck Pain
Ergonomic Setup
Position your screen at eye level, an arm’s length away. Your ears should sit directly above your shoulders when sitting upright. A monitor riser or laptop stand solves this for most desk workers immediately.
Screen Break Strategies
Follow the 20-20-20 rule: every 20 minutes, look at something 20 feet away for 20 seconds. Add a full posture reset every 30 minutes, stand, roll your shoulders back, and do 5 chin tucks.
Strengthening Exercises
Deep neck flexor training (chin tucks with progressive resistance) and lower trapezius activation exercises reduce long-term recurrence. Consistent training 3 times per week over 8 weeks produces measurable improvements in head position.
Sleep Position Optimization
Sleep on your back or side. Avoid sleeping on your stomach because it forces the neck to rotate 90 degrees for hours. Use a cervical pillow that supports the natural neck curve. Pillow height should keep your nose aligned with your sternum when lying on your side.
When to See a Doctor
See a doctor for neck pain at base of skull immediately if: the pain started after a head injury or fall, you have sudden severe pain described as the worst headache of your life, pain comes with fever and neck stiffness together (possible meningitis), you experience weakness or numbness in your arms or hands, or vision changes accompany the pain. Gradual worsening over weeks without a clear cause also warrants evaluation.
Frequently Asked Questions
What causes neck pain at the base of the skull?
Neck pain at base of skull most commonly comes from suboccipital muscle tightness, forward head posture, or C1-C2 joint stiffness. Occipital neuralgia causes electric, shooting pain specifically. The exact cause determines the correct fix, which is why most generic treatments fail.
How to relieve base of skull pain quickly?
To relieve base of skull pain fast, apply a heating pad for 15 minutes to the skull base, then do 10 chin tucks and a 30-second upper trapezius stretch on each side. This combination reduces suboccipital muscle tension within 20 minutes for tension-based cases.
Can screen time cause neck pain at the base of the skull?
Yes. Screen time and forward head posture pain is the leading cause in adults under 45. For every inch the head sits forward of the shoulder, the neck carries an extra 10 pounds of load. Four hours of forward head posture creates cumulative muscle overload that produces skull-base pain by evening.
Is stress responsible for neck tension pain?
Yes. Stress and muscle tension neck pain is physiologically real. Cortisol keeps neck and shoulder muscles in a semi-contracted state. Jaw clenching from stress loads the same suboccipital muscles. People under chronic stress have measurably higher muscle tone in the upper trapezius even at rest.
When is neck pain a serious problem?
Neck pain at base of skull becomes serious when it follows trauma, includes arm weakness or numbness, appears with fever and stiff neck together, or presents as a sudden explosive headache. These patterns require emergency evaluation for spinal injury, meningitis, or subarachnoid hemorrhage.
Can poor posture cause headaches from the neck?
Yes. Cervicogenic headache develops when C1-C2-C3 joint irritation refers pain upward through shared nerve pathways with the trigeminal nerve. It mimics a migraine but starts at the skull base and worsens with neck movement, not light or sound sensitivity.
How do I fix forward head posture?
Chin tucks 10 repetitions, 3 times daily, combined with lower trapezius strengthening and thoracic spine mobility work. A physiotherapist can confirm the degree of forward head posture and progress exercises appropriately. Postural change takes 8 to 12 weeks of consistent effort.
Should I see a doctor for neck pain?
See a doctor if neck pain at base of skull does not improve after 2 to 3 weeks of self-care, if pain radiates into the arm, or if occipital neuralgia symptoms appear. Persistent cervicogenic headache also needs physiotherapy assessment, not just painkillers.
About The Author

Medically reviewed by Dr. Chandril Chugh, MD, DM (Neurology)
Dr. Chandril Chugh is a U.S.-trained, board-certified neurologist with expertise in diagnosing and managing neurological disorders, including migraines, epilepsy, Parkinson’s disease, and movement disorders. His clinical focus includes evidence-based neurological care and patient education.
All content is reviewed for medical accuracy and aligned with current neurological guidelines.