Complex PTSD and sleep problems go together because trauma physically rewires the nervous system. The brain learns to stay on alert, and that alert state does not switch off at bedtime. Sleep requires the body to feel safe. A nervous system shaped by chronic trauma does not easily trust that safety.
The disruption is neurological. Understanding why trauma blocks sleep is the first step toward changing it. This article explains the biology, the specific sleep problems linked to Complex PTSD (C-PTSD), proven treatments, and practical tools for recovery.
Key Takeaways
- Complex PTSD and sleep problems are rooted in chronic hyperarousal (a state where the nervous system stays on high alert) and nervous system dysregulation.
- Nightmares in complex PTSD are common and directly connected to how the brain processes traumatic memories during sleep.
- Waking up multiple times with complex PTSD links to cortisol spikes (cortisol is the body’s stress hormone) and hypervigilance throughout the night.
- Complex PTSD and difficulty falling asleep often involve a fear of losing control or being vulnerable during sleep.
- Therapy for sleep issues in complex PTSD requires both trauma-focused therapy and specific sleep treatment working together.
Table of Contents
ToggleHow Complex PTSD Affects Sleep Regulation
Complex PTSD and sleep disruption begin in the brain and nervous system. This is not something you can fix by going to bed earlier or avoiding screens. The wiring itself has changed.
Hyperarousal and Sympathetic Nervous System Activation
The autonomic nervous system has two modes: the sympathetic system (fight or flight, which activates under threat) and the parasympathetic system (rest and digest, which allows calm).
In C-PTSD, the sympathetic system becomes chronically dominant. At bedtime, when sensory input reduces, the nervous system interprets quiet as dangerous rather than restful. Heart rate stays elevated, muscles stay tense, and the brain keeps scanning for threats.
Amygdala Overactivity During Sleep
The amygdala is the brain’s alarm center. In people with C-PTSD, it stays overactive even during sleep. Brain imaging research shows that trauma survivors show significantly higher amygdala activity during sleep compared to non-traumatized individuals. This overactivity is what triggers nightmares, sudden waking, and the feeling of dread upon waking even without a specific memory.
Cortisol Spikes and 3 AM Awakenings
Cortisol naturally peaks in early morning to prepare the body for waking. In C-PTSD, this cortisol spike happens too early and too sharply, often around 2am to 4am. The result is a sudden, wide-awake feeling in the middle of the night paired with racing thoughts, anxiety, and an inability to return to sleep.
Disrupted REM Sleep Processing
REM sleep (Rapid Eye Movement sleep) is when the brain processes emotional memories and reduces their emotional charge over time. In C-PTSD, REM sleep is fragmented and dysregulated. Traumatic memories do not get fully processed. Instead, they replay with full emotional intensity, which is what causes trauma-specific nightmares.
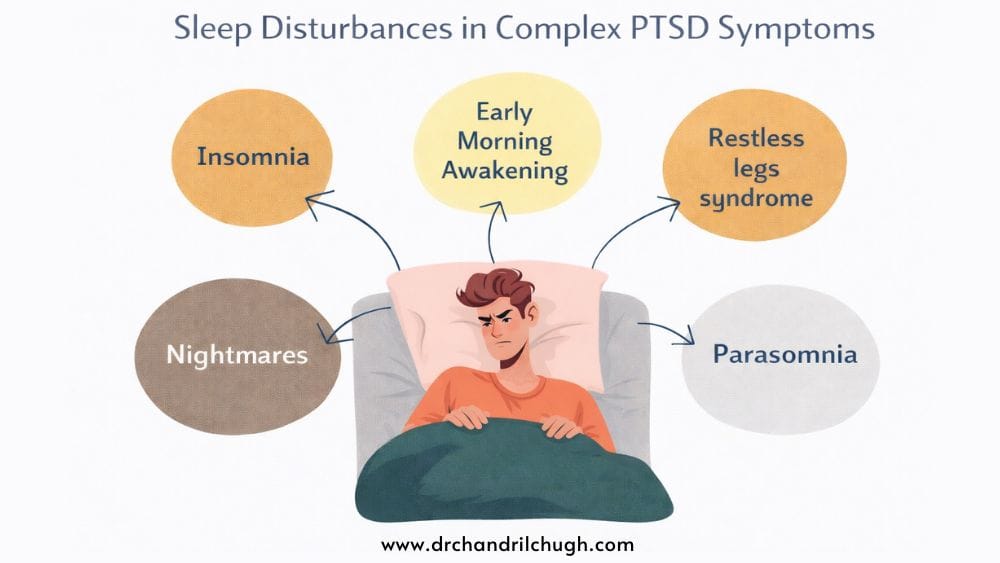
Sleep Disturbances in Complex PTSD Symptoms
Sleep disturbances in complex PTSD symptoms cover a wide range, and many people experience several at once rather than just one.
Insomnia
Insomnia in C-PTSD is not about racing thoughts about work or daily stress. It is fear-based. The brain resists sleep because sleep means a loss of conscious control and environmental monitoring. Falling asleep feels unsafe, not just difficult.
Fragmented Sleep
Fragmented sleep means waking multiple times throughout the night rather than sleeping in one continuous block. Each awakening is usually brief but fully activates the stress response, making return to sleep slow and difficult.
Non-Restorative Sleep
Non-restorative sleep means waking up after 7 to 8 hours feeling exhausted. This happens because the brain never reaches the deep slow-wave sleep stages needed for physical recovery. The nervous system stays in a light, vigilant state all night.
Early Morning Awakening
Waking between 3 am and 5 am and being unable to return to sleep is common in C-PTSD. This links directly to the abnormal cortisol spike pattern described above. People often describe it as being jolted awake by a feeling of dread rather than a sound or a specific nightmare.
Fear-Based Night Waking
Some waking episodes in C-PTSD are not triggered by dreams or sounds at all. They are triggered by the body’s own stress chemistry. A sudden surge of adrenaline (the emergency response hormone) can wake a person from sleep with no external cause, leaving them alert, shaking, and confused.
Nightmares in Complex PTSD
Nightmares in complex PTSD are one of the most distressing and least understood parts of the condition. They have a specific neurological cause.
Trauma Replay During REM Sleep
During REM sleep, the hippocampus (the brain’s memory filing system) and the amygdala work together to process stored experiences. In C-PTSD, this system is dysregulated. Instead of processing and filing traumatic memories with reduced emotional intensity, the brain replays them at full intensity. The nightmare is the replay.
Emotional Memory Reprocessing
Healthy REM sleep gradually strips the emotional charge from difficult memories. A distressing event becomes easier to recall without reliving it. In C-PTSD, this process breaks down. The emotional charge does not reduce. Each nightmare essentially refreshes the distress rather than reducing it.
Nightmares vs Night Terrors
Nightmares happen during REM sleep and are remembered after waking. Night terrors happen during deep non-REM sleep, cause intense physical responses like screaming or thrashing, and the person usually has no memory of them afterward. C-PTSD more commonly causes nightmares, though night terrors can also occur.
Physiological Stress Response After Waking
When you wake from a trauma nightmare, the body has been in a full threat response during the dream. After waking:
- Heart rate spikes sharply, sometimes reaching 100 to 130 beats per minute
- Sweating is common, often drenching
- Panic upon awakening includes disorientation, confusion about what is real, and a fear that the threat is physically present
- The physical stress response takes 20 to 40 minutes to fully calm down, making return to sleep very difficult
Waking Up Multiple Times with Complex PTSD
Waking up multiple times with complex PTSD is one of the most exhausting parts of the condition. It is the nervous system doing its job, wrongly applied to a context where there is no current threat.
Hypervigilance During Light Sleep
Hypervigilance (a state of being constantly on alert for danger) does not pause during sleep. During light sleep stages, the brain continues monitoring the environment. In C-PTSD, the threshold for deciding something requires waking is set extremely low. A door closing in another room, a change in temperature, or even a shift in the sleeping partner’s breathing can trigger full waking.
Environmental Sensitivity
Trauma-trained brains become highly attuned to environmental changes during sleep. Sounds, light changes, smells, and physical sensations that most people filter out automatically are flagged as potential threats. This is an adaptation from a period when those senses were genuinely needed for safety.
Startle Response at Night
The startle response (the physical jerk and spike of alarm triggered by sudden stimuli) is exaggerated in C-PTSD. During sleep transitions, which happen multiple times per night, small sounds or body twitches can trigger a full startle response that wakes the person completely.
Middle-of-the-Night Cortisol Release
Cortisol normally stays low in the middle of the night. In C-PTSD, the stress hormone system loses its normal rhythm. Cortisol can spike at 1am, 2am, or 3am, producing a wide-awake, anxious, heart-racing waking that clusters consistently around early morning hours. This is why, if you have C-PTSD, you wake up at the same time every night.
Complex PTSD and Difficulty Falling Asleep
Complex PTSD and difficulty falling asleep is a conflict between the body’s need for sleep and the nervous system’s interpretation of sleep as a threat.
Fear of Vulnerability
Sleep requires surrendering conscious control of the environment. For someone whose trauma involved situations where they had no control or protection, this surrender is genuinely frightening. Lying in the dark waiting for sleep can feel identical to the helplessness experienced during trauma.
Racing Thoughts and Rumination
At bedtime, external distractions disappear. Intrusive thoughts, which the brain can suppress during daytime activity, surface more forcefully at night. These are not general worries. They are often specific trauma-related memories, fragmented images, or looping thought patterns connected to past events.
Intrusive Memories at Bedtime
Intrusive memories (involuntary flashbacks or sensory memories linked to trauma) are more frequent at sleep onset when the brain shifts from beta waves (active thinking) to alpha and theta waves (drowsy states). This wave transition seems to open access to deeply encoded trauma memories.
Bedtime Avoidance Patterns
Many people with C-PTSD develop unconscious delay tactics at night: staying up very late, sleeping with the television on, avoiding the bedroom until extreme exhaustion forces sleep. These patterns are the nervous system’s attempt to reduce the period of vulnerability before sleep.
Therapy for Sleep Issues in Complex PTSD
Therapy for sleep issues in complex PTSD works best when trauma treatment and sleep treatment are combined. Treating only one does not fully resolve the other.
Trauma-Focused CBT
Trauma-Focused Cognitive Behavioral Therapy (TF-CBT) addresses the distorted thought patterns and fear responses that keep the nervous system in a threat state. By processing the trauma cognitions, the brain gradually reduces the threat response at bedtime.
EMDR and Sleep Improvement
Eye Movement Desensitization and Reprocessing (EMDR) is a structured therapy that uses bilateral stimulation (guided eye movements or tapping) to help the brain reprocess traumatic memories. As traumatic memories lose their emotional charge through EMDR, nightmare frequency and intensity reduce measurably, often within 6 to 12 sessions.
CBT-I (Cognitive Behavioral Therapy for Insomnia)
CBT-I is a structured program targeting the specific thought patterns and behaviors that maintain insomnia. It includes sleep restriction therapy, stimulus control (rebuilding the mental association between bed and sleep), and cognitive restructuring of sleep-related fears. CBT-I is recommended as a first-line treatment for insomnia by the American College of Physicians, and it adapts well to trauma contexts.
Imagery Rehearsal Therapy for Nightmares
Imagery Rehearsal Therapy (IRT) is a technique specifically for trauma nightmares. The person writes down a recurring nightmare, changes the ending to something neutral or positive while awake, and then mentally rehearses the new version. Over 3 to 6 weeks, the brain begins replacing the traumatic dream content with the rehearsed version. IRT shows strong results for reducing nightmare frequency in PTSD.
Medication Considerations (When Necessary)
Doctors sometimes prescribe prazosin (a blood pressure medication that also reduces nightmare frequency in PTSD) when nightmares are severe. Dosage varies by individual. Some clinicians also use low-dose medications to support sleep initiation. Medication alone does not resolve the underlying trauma response and works best alongside therapy.
Self-Management Strategies That Support Recovery
Nervous System Regulation Before Bed
Spend 20 to 30 minutes before bed in deliberate parasympathetic (calming) activities. Progressive muscle relaxation (tensing and releasing muscle groups from feet to face) reduces the physical tension that keeps the sympathetic nervous system active. Warm baths raise and then drop core body temperature, triggering natural sleepiness.
Safe Bedtime Environment Design
Reduce environmental triggers. Blackout curtains, consistent white noise, and a room temperature between 18 and 20 degrees Celsius (64 to 68 Fahrenheit) reduce the number of stimuli the hypervigilant brain has to monitor. Sleeping with a weighted blanket provides deep pressure stimulation that activates the calming vagal nerve pathway.
Grounding Techniques for Night Awakenings
After waking from a nightmare or anxiety-based waking, use the 5-4-3-2-1 grounding technique: identify 5 things you can see, 4 you can touch, 3 you can hear, 2 you can smell, and 1 you can taste. This technique reorients the brain to the present and out of the threat memory.
Controlled Breathing for Hyperarousal
Box breathing (inhale for 4 counts, hold for 4, exhale for 4, hold for 4) activates the vagus nerve (the main nerve of the parasympathetic system) within 2 to 3 minutes. Extended exhale breathing (inhale for 4, exhale for 6 to 8) is even more effective for reducing heart rate rapidly after a nightmare.
Gradual Exposure to Darkness
If darkness itself is a trigger, start with a very low-level nightlight and reduce it incrementally over several weeks. Forcing total darkness before the nervous system is ready will increase waking. Gradual exposure lets the brain update its threat assessment at a pace it can tolerate.
Long-Term Impact of Untreated Sleep Disturbance in Complex PTSD
Leaving complex PTSD and sleep disturbances untreated has consequences that extend far beyond feeling tired.
Emotional Dysregulation
Sleep deprivation impairs the prefrontal cortex (the part of the brain that regulates emotional responses). When sleep is consistently poor, emotional flashbacks, irritability, and sudden intense reactions become harder to control. This creates a cycle where sleep loss worsens C-PTSD symptoms and C-PTSD symptoms worsen sleep loss.
Increased Anxiety and Depression
Chronic sleep deprivation raises cortisol levels persistently. Elevated cortisol over weeks and months increases the risk of anxiety disorders and clinical depression, both of which are already elevated in C-PTSD.
Memory and Concentration Impairment
The hippocampus consolidates (stores) new memories during sleep. Without adequate sleep, memory formation weakens. People describe brain fog, difficulty retaining new information, and an inability to concentrate, which also affects therapy engagement and daily functioning.
Cardiovascular Stress
Repeatedly elevated cortisol and adrenaline at night raise blood pressure and resting heart rate over time. Long-term untreated sleep disruption in C-PTSD increases cardiovascular risk in the same way chronic stress does.
Delayed Trauma Recovery
Therapy for C-PTSD requires the brain to process, reframe, and store new emotional information. That processing happens largely during REM sleep. Without adequate REM sleep, the gains made in therapy sessions do not consolidate as effectively. Untreated sleep disruption literally slows the pace of trauma recovery.
FAQs
Does complex PTSD cause sleep problems?
Yes. Complex PTSD and sleep problems are directly linked through chronic hyperarousal, cortisol dysregulation, and amygdala overactivity. Over 70% of people with C-PTSD report significant sleep disturbances, including insomnia, nightmares, and non-restorative sleep.
Why do nightmares happen in complex PTSD?
Nightmares in complex PTSD occur because the brain’s REM sleep memory-processing system is dysregulated. Instead of reducing the emotional charge of traumatic memories over time, the brain replays them at full intensity each night. Each nightmare refreshes the distress rather than resolving it.
Why do I wake up multiple times with complex PTSD?
Waking up multiple times with complex PTSD happens because the stress hormone system loses its normal rhythm. Cortisol spikes around 2am to 4am instead of staying low, producing a sudden wide-awake response. Hypervigilance also lowers the waking threshold so minor sounds trigger full arousal.
Can complex PTSD cause difficulty falling asleep?
Yes. Complex PTSD and difficulty falling asleep is rooted in the brain interpreting sleep itself as a threat. Losing conscious control feels identical neurologically to the helplessness felt during trauma. This triggers the same fight-or-flight response that blocks sleep at the physiological level.
What therapy helps sleep issues in complex PTSD?
Therapy for sleep issues in complex PTSD combines EMDR for trauma memory reprocessing, CBT-I for insomnia behaviors, and Imagery Rehearsal Therapy specifically for nightmares. Using only one approach without the others leaves part of the problem untreated and slows full recovery.
Is insomnia common in complex PTSD?
Yes. Insomnia is one of the most consistent sleep disturbances in complex PTSD symptoms. It affects the ability to fall asleep, stay asleep, and feel rested after sleeping. Unlike regular insomnia, trauma-based insomnia requires trauma-informed treatment to resolve effectively.
Can REM sleep be disrupted in CPTSD?
Yes. REM sleep is severely disrupted in C-PTSD. The amygdala remains overactive during REM, trauma memories replay without emotional processing, and the normal memory consolidation function of REM is compromised. This is why complex PTSD and sleep treatment must address REM specifically through approaches like EMDR and IRT.
How can I calm hyperarousal before bed?
Box breathing for 5 minutes (4 counts in, 4 hold, 4 out, 4 hold) activates the vagus nerve and lowers heart rate measurably. Progressive muscle relaxation for 10 minutes reduces physical tension. Both work within one session, not after weeks of practice.
Does CBT-I work for trauma-related insomnia?
Yes, but it works better when combined with trauma therapy. CBT-I alone addresses sleep behaviors and sleep-related thoughts effectively. Without addressing the underlying trauma response, the fear of sleep and the hyperarousal that feeds insomnia persist. Combined CBT-I and trauma therapy shows stronger outcomes than either alone.
When should I seek help for CPTSD-related sleep problems?
Seek help when sleep disruption is happening more than 3 nights per week, lasting longer than 4 weeks, or causing impairment in daily functioning. Also seek help immediately if nightmares are becoming more frequent, waking you more than twice per night, or causing you to avoid sleep entirely.
About The Author

Medically reviewed by Dr. Chandril Chugh, MD, DM (Neurology)
Dr. Chandril Chugh is a U.S.-trained, board-certified neurologist with expertise in diagnosing and managing neurological disorders, including migraines, epilepsy, Parkinson’s disease, and movement disorders. His clinical focus includes evidence-based neurological care and patient education.
All content is reviewed for medical accuracy and aligned with current neurological guidelines.